Table of Contents
Radical nephrectomy is the removal of the whole kidney and the surrounding fatty tissue. It is done when it is not possible to leave a functioning kidney behind after a partial nephrectomy. It is generally recommended for kidney cancers that have not yet spread but that have grown into surrounding tissue. It is also used for stage I tumours when partial nephrectomy is not an option. Most people can live with only one functioning kidney without major complications.
How is radical nephrectomy performed?
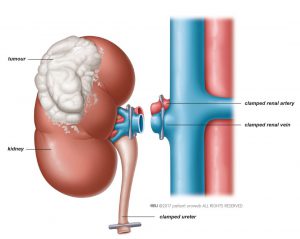
You will be asleep (general anaesthesia) for radical nephrectomy. To begin, the size of the tumour is determined. To prevent tumour spillage, the surgeon keeps your kidney covered with a protective layer of fatty tissue. The surgeon then separates the renal artery, renal vein, and ureter from the kidney (Fig. 1). Finally, the kidney is removed.
Lymph-node removal
If you have enlarged lymph nodes, the urologist may decide to remove them in a procedure called lymphadenectomy. In some cases, the CT scan has shown that lymph nodes are enlarged, thus possibly involved, and the doctor will discuss possible treatment with you. In other cases, the urologist detects enlarged lymph nodes during surgery and may decide to remove them.
Removal of the adrenal gland
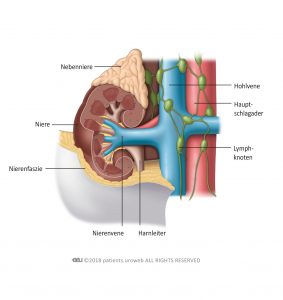
The adrenal gland is an organ located on top of each kidney (Fig. 2). It produces stress and steroid hormones. If the tumour has spread to the adrenal gland, the gland needs to be removed together with the kidney. This procedure is known as adrenalectomy. A CT scan before surgery can confirm that the tumour has spread to the adrenal gland. In other cases, the urologist detects tumour cells in the adrenal gland during surgery and will remove it. The remaining healthy adrenal gland continues to produce all the hormones needed.
Surgical approach
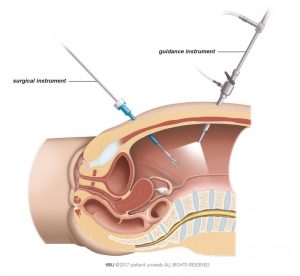
Radical nephrectomy can be performed two ways, and both are equally effective. The operation can be done through a cut in the abdominal wall to reach the kidney and the tumour directly (open surgery). It can also be done with tube-like instruments placed through small cuts to see inside the body (laparoscopic surgery) (Fig. 3). Laparoscopic surgery can also be done assisted by a surgical robot system.
Laparoscopic surgery generally leads to faster recovery than open surgery, but the technique is demanding and your doctor needs to have experience doing this type of surgery. Open radical nephrectomy may be recommended in certain medical cases or if laparoscopic surgery is not available in your hospital. The open approach has a longer recovery time, and there is higher risk of pain and complications after surgery compared with laparoscopy.
What are the side effects of the procedure?
Usually, you can leave the hospital between 3 and 7 days after surgery. The length of hospital stay can vary in different countries. You may experience minor pain in the side of your body for some weeks after open radical nephrectomy.
You need to go to your doctor or go back to the hospital right away if you:
- Develop a fever
- Have heavy blood loss or pain
What is the impact of the treatment?
Radical nephrectomy is a common procedure for kidney cancer that has not spread to other tissue. Most patients are cancer-free up to 5 years after surgery. Because you are left with only one functioning kidney, you have a higher risk of chronic kidney disease than if you had both. Reduced kidney function is also a risk factor for cardiovascular disease.
What will the follow-up be like?
After radical nephrectomy for kidney cancer, your doctor will plan regular follow-up visits with you. How often these visits are needed depends on analysis of the removed tumour. Follow-up visits will continue for at least 5 years. Common tests during follow-up visits are imaging of the abdomen (CT scans and ultrasound), chest x-ray, and urine and blood analyses.
Surgery after recurrence
If a recurrence is detected during follow-up, you may need additional surgery. Before this surgery your doctor may recommend to shrink the tumour with antiangiogenic therapy . It is also possible that your doctor recommends this therapy or ablation therapy after surgery.