Table of Contents
Ureteroscopy
This information provides you with the essentials on the treatment ureteroscopy. It also contains an animation that shows what happens when you undergo a ureteroscopy as well as answers to the most frequently asked questions.
What is ureteroscopy?
Ureteroscopy (URS) is a preferred method for the treatment of small- to medium-sized kidney stones located in any part of the urinary tract.
The procedure
- The procedure is typically performed with the patient under general anaesthesia (asleep).
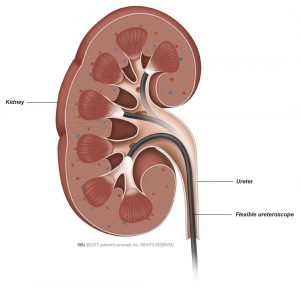
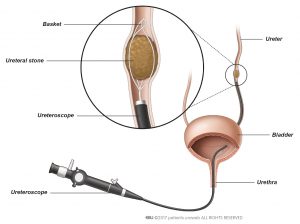
- During this procedure, a ureteroscope is inserted through the urethra and bladder into the ureter (a tube that carries urine from the kidneys to the bladder) or kidney.
- X-ray images with a contrast agent (dye) in the ureters may be used to allow the urologist to see where the stone is located and to rule out other abnormalities.
- The ureteroscope is long and thin with a tiny fibre optic camera at the end that is used to see beyond the bladder into the ureters.
- Once the stone is located, it is pulled out directly with a “stone basket” or a laser is used to break the stone into smaller pieces before they are extracted using the basket.
Some ureteroscopes are flexible like a thin, long straw. Others are more rigid and firm.
Preparation for the procedure
Always ask your doctor about the treatment-steps and any special instructions, as these can differ per hospital and country.
Instructions may include:
- When to stop certain medications, such as blood thinners.
- When to empty the bladder before the procedure.
- When to arrange pain medication after the procedure (if necessary). Discuss this early with your nurse and/or doctor.
- Arranging a ride home after your hospital discharge.
- Not to eat, drink, or smoke for approximately 6-8 hours before the procedure to prepare for the anaesthesia.
Before surgery, someone from your health care team, usually the anaesthesiologist, will assess which method of anaesthesia is appropriate for you.
Depending on the country you live in and your hospital, methods of anaesthesia can include:
- General anaesthesia
- An epidural (an anaesthetic used to numb the lower half of the body) with or without sedation
You may be asked to give a urine sample before the procedure to test for a urinary tract infection.
Medical team
It is important that, aside from the doctor and nurses in the hospital who are responsible for your treatment, your general practitioner and other caregivers who you are in contact with, are informed about your treatment.
Support and questions
It can help and make you feel more comfortable if your partner, relatives or friends have read the information regarding the procedure. Write down all of your questions to remind you of any important points you need to ask from your doctor or nurse.
Let someone accompany you to an appointment to help you remember any questions you may need to ask.
The operation
This animation shows what happens when you undergo a ureteroscopy.
The procedure in this animation is performed with a flexible ureteroscope. As the name suggests, the end of the instrument is flexible so it can access areas within the kidney that are otherwise difficult to reach.
What to expect after the procedure
In some patients, a temporary small tube, called a stent, is placed in the ureter (Fig. 2). This stent facilitates urine flow to the bladder as the ureter can be swollen after the procedure.
After surgery you may have a urine catheter. This is a tube that is placed through the urethra into the bladder. The catheter allows urine to drain from the bladder. You will also carry an infusion that helps you to regulate the fluid in your body.
Depending on management of the hospital, you will either proceed to the recovery room or your own room after treatment. You will be regularly checked for your blood pressure, heart rate and pain. Ask your nurse about visiting hours for friends and relatives.
The urine catheter and/or stent are usually removed shortly after the procedure. You can leave the hospital if you are able to empty your bladder sufficiently and you have no fever or too much pain.
You may feel mild to moderate pain in your lower abdomen and you may have a strong urge to urinate. These symptoms are usually the result of the inserted catheter and/or stent. There is medication available to treat these symptoms, do not hesitate to ask.

What to expect back home
Your doctor or nurse will provide discharge instructions for rest, driving, and physical activities after the procedure.
If a JJ-stent was placed during the procedure and is not taken out before your hospital discharge, your doctor will advise you when it needs to be removed. This can take anywhere between several days and a few weeks.
Because instruments were inserted into your urinary tract, you may experience several urinary symptoms for some time after surgery. These problems usually disappear in a few weeks.
Symptoms may include:
- A mild burning feeling when urinating
- Small amounts of blood in the urine
- Mild discomfort in the bladder area or kidney area when urinating
- Need to urinate more frequently or urgently
- Pain resulting from an internal abrasion that needs time to heal
Try to drink often, but in small quantities. Sometimes a blood clot can cause pain (colic). The urine contains a substance urokinase which will dissolve this clot.
If the pain remains despite pain killers, contact the hospital or your doctor.
What can I do the first week after surgery?
- Try to drink enough fluids: 1.5 liters daily (in small quantities) throughout the day to facilitate urine flow and the spontaneous loss of small stone fragments
- Try not to have sex within the first week after the procedure to avoid urinary tract infections
- Eat more vegetables and less meat to have a softer stool – if you do not have to squeeze during the toilet visit it will aid the inner healing process
Give your body a rest during the first week after the procedure – you are allowed to lift maximum 5 kg and go for walks. You can start cycling and exercising after this period.
When should I call the hospital or my general practitioner?
- When you have a fever above 38.5 degrees
- When you experience a serious burning sensation (not mild) when urinating
- When you are unable to urinate
- When you see large amounts of blood in your urine, which is not relieved by rest or hydration
- When you continue to have severe pain in your side, despite painkillers
You should tell your doctor right away if bleeding or pain is severe or if problems last longer or worsen after you have been discharged.
Your doctor may prescribe an antibiotic to treat or prevent an infection or relieve your pain. You should report any signs of infection––including severe pain, chills, or fever—to your doctor right away.
Follow-up
A follow-up appointment will be scheduled before you leave the hospital. Follow-up may include:
- Discussing laboratory results
- Ultrasound or X-rays check
- Double-J stent removal
Laboratory results
The removed stone is sent to the laboratory to determine its composition. This may take several weeks. Based on the laboratory results, along with blood and urine tests taken prior to treatment, your doctor is able to determine if you are at high risk of forming new stones (recurrence).
Ultrasound or X-rays check
Your doctor may also do an ultrasound or X-ray examination to check for any stones that may be left and to make sure that there is good passage of urine from the kidney to the bladder.
Double-J stent
The removal of a double-J stent generally takes less than a couple of minutes. You may feel mild to moderate pain in your lower abdomen, and you may have a strong urge to urinate. These symptoms are usually caused by the inserted stent. Medication is available to treat these symptoms. Do ask your doctor.
Changes in your lifestyle
Even if you have a low risk of forming another stone, your doctor and nurse will advise you to make some lifestyle changes.
Lifestyle changes may include:
- Increasing fluid intake to 2.5-3.0 litres per day to pH of your urine
- Adopting a balanced diet, with less meat and alcohol and more vegetables and fibre to have healthy calcium levels and less intake of animal proteins
- Maintaining a healthy weight (normal body mass index) and adequate physical activity
What if the doctor suspects that I have a high risk of forming new stones?
If the results show that you have a high risk of forming more stones, your doctor will do a metabolic evaluation. This is a series of blood and urine tests to determine the possible causes of your stone formation. Depending on the test results, your doctor will recommend preventive measures or further tests. Besides changes in your lifestyle, you may also be advised to take medication, that reduces the risk of stones recurring. Generally, the medication will cause little to no side effects.