Table of Contents
Sling implantation
Sling implantation aims to cure stress urinary incontinence (SUI) by compressing the urethra or repositioning the urethra in relation to the bladder neck with a specific material. By doing this, they support the pelvic floor muscles and increase resistance to the pressure of a full bladder. The goal of both techniques is to prevent urine leakage.
Different types of sling operations are available. These differences include:
- Surgical approach: retropubic or transobturator insertion
- Material: synthetic or biological
- Shape: two-armed, four-armed, and adjustable slings
Which type of sling is recommended for you depends on your individual situation and needs. It also depends on the availability of different types of slings in your hospital and your surgeon’s experience with them.
When should I consider a sling?
Slings can be considered in case of mild to moderate urinary stress incontinence. They are also recommended when other surgical treatments are not possible, or if you do not want to undergo major surgery.
A sling may be a option after other procedures have failed.
Each type of sling has specific characteristics, results, and possible complications. Ask your doctor about his or her experience with the sling suggested to you.
How are slings implanted?
You will typically be asleep (general anaesthesia) for this procedure. Spinal anaesthesia can also be used to block nerve response to pain.
Steps:
- The bladder is emptied. The surgeon inserts a catheter to make sure that your bladder is completely empty during surgery.
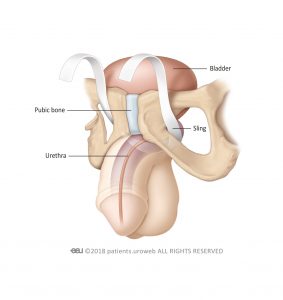
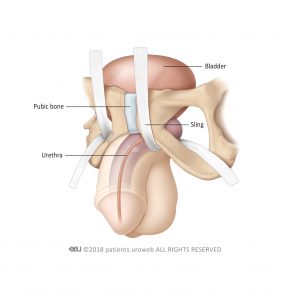
- An incision is made between the scrotum and the anus to insert the sling. In two-armed slings, the ends of the sling are put in position on both sides of the urethra, shaping the sling like a hammock. Then, the ends of the sling are attached to tissue either just above the pubic bone, or around the groin. In four-armed slings, two ends of the sling are attached to the groin, while two others are attacted to tissue around the pubic bone.
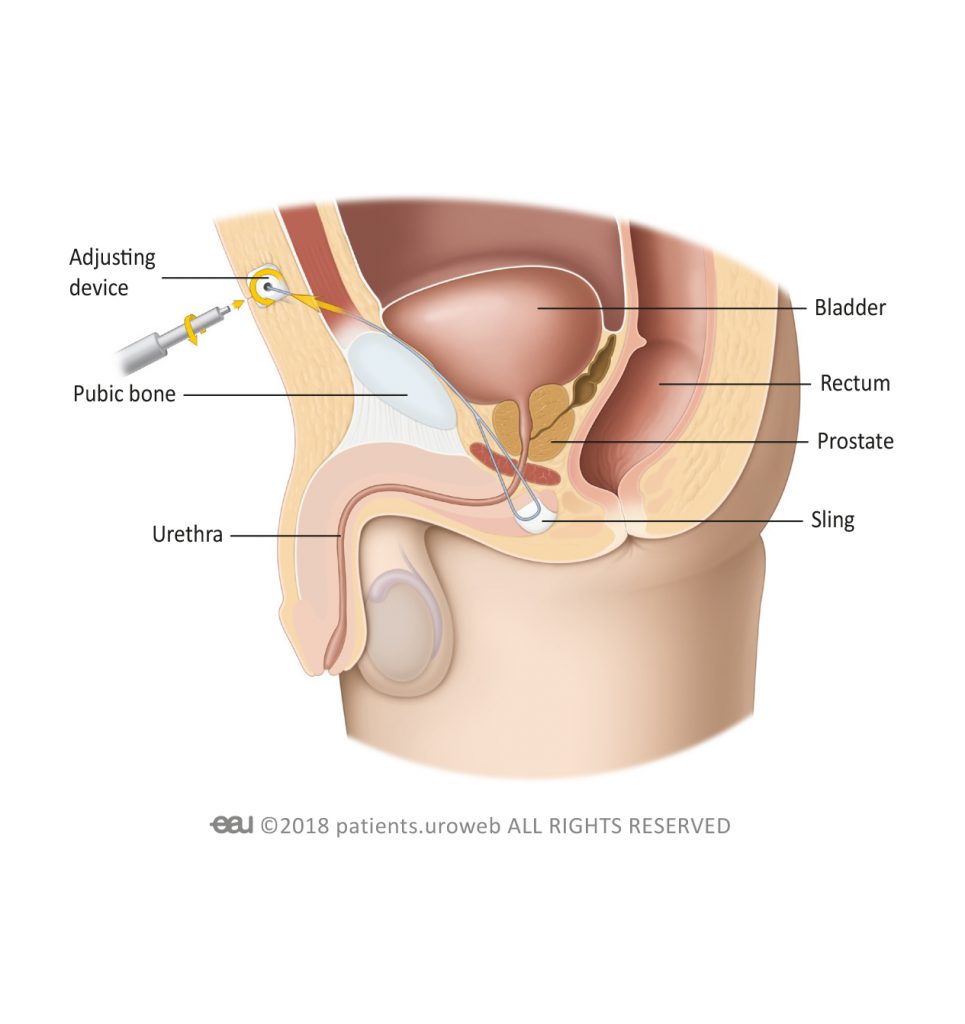
- For adjustable slings, the technique may include additional incisions to insert an adjusting device in the body.
How do I prepare for the procedure?
Before surgery, the doctor will ask for a urine sample. This will be tested to make sure you do not have a urinary tract infection. If you have an infection, this should be treated with antibiotics before scheduling the surgery. Your doctor may prescribe antibiotics before, during, and after the operation even if there is no infection, for the sake of prevening any infections.
Your doctor will advise you in detail about how to prepare for the procedure. If you need general anaesthesia, you must not eat, drink, or smoke for a certain time period before surgery. If you are taking any prescribed medication, discuss it with your doctor. You may need to stop taking it several days before surgery. Your doctor will advise you on when you can start taking it again.
How long will it take me to get back to my daily activities?
The doctor will generally remove the catheter within 24 hours after the surgery and monitor your recovery. Usually, you can leave the hospital a few days after the procedure. If you have problems urinating or there is much post-void residual urine in the bladder, you may have to stay longer. The recommended length of hospital stay varies in different countries.
After any surgery, your body needs time to fully recover. It can take up to 6 weeks for the wound to completely heal. During this time you may experience pain in the pelvic area, or feel pain when you urinate. Your doctor can prescribe medication to deal with these symptoms.
Your wound will be checked as well. Usually, stitches that dissolve and disappear are used.
During the recovery period your doctor may recommend to:
- Consume enough liquid, especially water, to provide at least 2 litres of urine output
- Do not lift anything heavier than 5 kilograms
- Do not do any heavy exercise
- Take showers instead of baths
- Avoid thermal baths, or going to the sauna
- Prevent constipation by adapting your diet
- Avoid sexual activity
- Avoid activities which can traumatise the operation site, such as cycling and horseback riding.
Call your doctor or go back to the hospital right away if you:
- Have a fever
- Are unable to urinate
- Have heavy blood loss or pain
- Notice the wound starts to bleed or leak transparent fluid, or it hurts
- Notice swelling, pain, or redness in the scrotum