Table of Contents
What is a neurourological disorder?
The nervous system connects the brain and spinal cord to all parts of the body through a network of nerves. A disturbance in that network can cause problems storing and passing urine. Urinary problems caused by the nervous system are called neurourological disorders.
What is neurogenic lower urinary tract dysfunction?
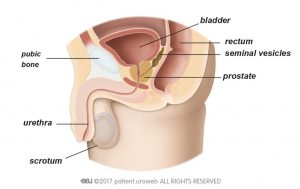
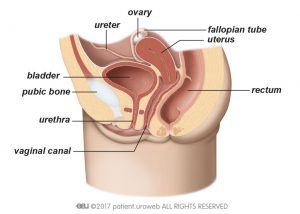
The lower urinary tract consists of the bladder and urethra and includes the prostate in men (Figures 1a and 1b). The bladder stores the urine produced by the kidneys. It is a hollow stretchy bag made of muscle tissue that sits on the pelvic floor muscles. Normally the bladder is able to store urine without building up high pressure. Below the bladder, the urinary sphincter helps store the urine and prevent leakage. It is composed of different parts and muscle layers. The urethra is the tube through which urine passes from the bladder out of the body.
The main functions of the lower urinary tract are storing and passing urine. Both functions are regulated by the nervous system, which coordinates interaction of the bladder and the sphincter. For normal storage, the bladder muscle should be relaxed and the sphincter muscles tense. For urination, the bladder muscle should contract to build up pressure and to press the urine out, and the sphincter should relax to allow for easy and complete emptying without resistance.
These functions involve many parts of the nervous system, including the brain, the spinal cord, and the peripheral nerves. Any disturbance of these parts can lead to malfunction of normal storage and voiding and cause many symptoms. This disturbance is called neurogenic lower urinary tract dysfunction.
You may have a neurogenic lower urinary tract dysfunction if you also have one or more of the following conditions:
- A neurologic disease such as dementia, stroke, or multiple sclerosis
- Previous surgery or injury to the spine or pelvis
- Previous radiation
- Deformity of the spine
- A slipped disc
- A brain tumour or abnormal cell growth that affects the nervous system
- Diabetes
- Numbness or pain in the hands or feet (called peripheral neuropathy)
Symptoms and complications of neurogenic lower urinary tract dysfunction
Symptoms and complications of neurogenic lower urinary tract dysfunction depend on where the problem is in the nervous system. Maybe you’ve noticed that normal storage and passing of urine is disrupted. Sometimes a problem doesn’t cause any discomfort.
Symptoms include:
- Slow or incomplete emptying of the bladder
- No sensation of the bladder
- Feeling abdominal fullness
- Not knowing when or if you will urinate (bladder spasticity)
- A frequent and compelling urge to empty the bladder, day or night, that is difficult to defer
- Incontinence
- Pain in the bladder or genital region
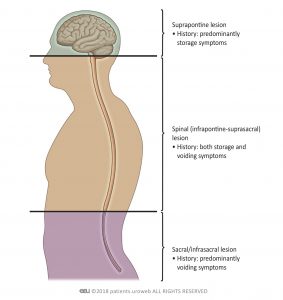
The location of the neurological problem usually influences the type of symptoms the patient may experience, for example: storage symptoms, urinary urgency or voiding symptoms, such as a weak urinary stream (Figure 2). Urological problems that occur after sudden changes like spinal injury tend to be more severe than those caused by chronic conditions.
Complications
Neurogenic lower urinary tract dysfunction can cause a variety of short- or long-term complications:
- Damaged kidney function caused by high pressure in the bladder is the most significant complication.
- The bladder can deteriorate and lose the ability to empty if high pressure builds up during storage or urination.
- Incomplete emptying of the bladder or backflow of urine to the kidneys might cause recurrent urinary tract infections, which can lead to dangerous effects on organs or even the whole body.
Delay of treatment might lead to worsening of all lower urinary tract function. This results in the need for more drastic therapy. Generally, treatment and follow-up examinations are based on the type of neuro-urological disorder and the underlying cause.
Diagnosis of neurourological disorders
Early diagnosis and treatment are essential in neurourological disorders. Early intervention can prevent irreversible changes of the lower and upper urinary tract.
When diagnosing neurourological symptoms, your doctor may:
- Take a thorough medical history
- Ask you to keep a bladder diary
- Ask you to complete a quality-of-life questionnaire
- Do a physical examination
- Test how your bladder fills and empties with pressure measurements (urodynamics)
- Check your kidney function
Medical history
The medical history is the cornerstone of evaluation. The answers will help determine diagnosis and treatment options.
Your doctor will ask you about past and present symptoms and illnesses. Your doctor also might want to know all medications you are taking regularly. The questions may address urinary and bowel symptoms as well as sexual function. Patients with neuro-urological symptoms may have related bowel and sexual problems.
Bladder diary
Your doctor may ask you to keep a bladder diary. You will be asked to document the number of times you urinated, the volume of urine passed, pad weight if you are using pads, and incontinence and urgency episodes. This is typically done over 24 hours and for 3 consecutive days to help identify the problem.
Quality-of-life questionnaire
Your doctor may ask you to fill out several questionnaires to assess your present and future quality of life. This aspect is important to monitor the effect of your therapy.
Physical examination
Your doctor may also do a thorough physical examination. The examination test all sensations and reflexes in the urogenital area as well as the anal sphincter and pelvic floor functions. This information is needed to understand later diagnostic tests.
Your doctor may also decide to analyse your urine and blood chemistry. Ultrasound or other imaging techniques may be recommended to evaluate the urinary tract.
Urodynamics
Urodynamic tests help your doctor to assess the function of your bladder.
Treatment of neurourological disorders
If you have a neuro-urological problem, the main goal is to protect your kidneys and ureters. These organs compose the upper urinary tract.
Kidney failure may result from many neurological conditions, for instance, spinal cord injuries. Your urologist may suggest a treatment to protect your kidney function even if you don’t have bothersome symptoms.
Provided that your kidneys are safe, priorities in neuro-urology treatment are:
- Restoring the normal function of the bladder
- Achieving or maintaining continence to improve quality of life
General information about neurourological disorders
Urinary tract infection in neurourological patients
Urinary tract infection (UTI) is diagnosed with common signs and/or symptoms:
- Strong urge to urinate that doesn’t go away
- Burning sensation or discomfort when urinating (dysuria)
- Passing frequent, small amounts of urine
- Cloudy urine with increased urine odour
- Pink, red, or brownish urine
- Pain above the pubic bone in women
Laboratory findings like a lot of bacteria or white blood cells in the urine confirm the diagnosis.
In neuro-urological patients, UTI can be caused by:
- Weakened defence mechanisms
- Inability to empty the bladder completely
- Catheterisation
Asymptomatic bacteriuria is the presence of bacteria in the urine without symptoms. It is much more common in patients with spinal cord injury than in the general population. The condition varies depending on bladder management—for example, clean intermittent catheterisation or an indwelling catheter. It should not be routinely screened for or treated in patients with neuro-urological disorder.
If you have a symptomatic UTI, you may have other signs and symptoms in addition to or instead of traditional signs and symptoms of a UTI:
- Fever
- Incontinence
- Unpredictable need to urinate
- Malaise
- Lethargy or sense of unease
- Discomfort or pain over the kidney or bladder
- Sudden occurrence of high blood pressure (autonomic dysreflexia)
If a symptomatic UTI is present, your doctor wmay do a urinalysis and take a urine culture to identify the bacteria involved.
Treatment asymptomatic bacteriuria
Treating asymptomatic bacteriuria does not have a urological effect but causes many more resistant bacterial strains to develop. For this reason, it should not be treated in patients with neuro-urological disorders.
Sexual (Dys)function and fertility
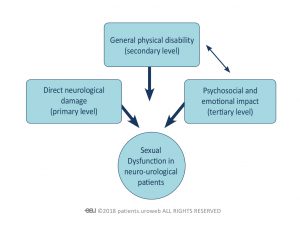
Neuro-urological disease affects patients’ sexual lives physically, psychologically, and sensory (Figure 3). A negative effect may be caused by direct impairment of the nerves that signal the pelvic and genital area. The psychosocial and emotional impact of neuro-urological disease can also be negative and must be addressed along with other causes.
Multidisciplinary teams should be available to address the different aspects of sexual dysfunction in neuro-urological patients.
Male fertility
Male neurological patients often have a combination of erectile dysfunction, ejaculation disorder, and impaired sperm quality. This combination causes decreased fertility. If you want to father a child and it is not possible naturally, sperm can be collected for later use in assisted reproduction. In men with spinal cord injury, especially of the thoracic spine (Th6 disc or above), sudden high blood pressure (autonomic dysreflexia) might occur during sexual activity and ejaculation. If you have a spinal cord injury, you should keep this in mind and tell the staff at your fertility clinic.
Some men have retrograde ejaculation, which causes sperm to go inside the bladder during ejaculation instead of out of the penis. It can be reversed using specific drugs or a balloon that prevents sperm going to the bladder.
Different techniques can be used to collect sperm from men with spinal cord injury.
Techniques like prostatic massage or stimulation with a vibrator may be used for sperm collection. Transrectal electroejaculation uses a light electrical current to cause ejaculation while the patient is asleep under anaesthesia, but it yields less viable sperm.
If these techniques do not work, sperm can be collected through microsurgery of the tube that carries sperm from the testicles (epididymis) or surgical removal of testicular pulp.
Intracytoplasmic sperm injection is an assisted reproductive technology. Since its introduction, spinal cord injury patients have a good chance of becoming biological fathers regardless of the technique used to collect sperm.
Female sexuality
Most of the information available is from women with spinal cord injury and multiple sclerosis. Several areas of sexual life are frequently impaired in neuro-urological female patients, such as sexual desire, lubrication, and orgasm. Most women continue to be sexually active but show decreased satisfaction levels.
Female fertility
Women with spinal cord injury may have a short period without menstruation (about 6 months) immediately after the injury. However, many are able to become pregnant once menstruation returns.
Special care must be taken during labour and delivery because complications can occur such as bladder problems, spasticity, pressure sores, anaemia, and sudden high blood pressure (autonomic dysreflexia).
Living with a neurourological disorder
Many characteristics, symptoms, and hazards of neuro-urological disorders depend on the underlying cause. It’s possible that you are not bothered by symptoms but have a risk of developing complications. A timely and thorough diagnostic evaluation helps prevent worsening of the situation.
Many treatment options enable individualised therapy. Safety and quality of life are the main goals of therapy, with kidney function being the main aspect of safety.
Protect your kidneys
Depending on the characteristics, a neuro-urological disorder can lead to kidney problems. This is serious and might lead to intensive, time-consuming treatment, reduced quality of life, and early death.
The primary aim of treating neuro-urological disorders is the conservation of kidney function. Therapeutic measures like catheterisation may substantially reduce your quality of life but prevent even more serious problems. If your doctor’s treatment advice seems unreasonable to you, you should discuss your concerns and ask for alternatives.
Depending on the characteristic of your neuro-urological disorder, your doctor might want to check your kidney function regularly. Your family doctor should be informed and should look for signs of kidney problems.
Manage symptoms
Neurourological disorders are often unstable. The symptoms may vary widely, even within a relatively short time period. Regular follow-up with your doctor is necessary. How often depends on the underlying cause.
Urinary incontinence may significantly affect your social life. Many treatment options exist. You shouldn’t be embarrassed to discuss your situation with your doctor.
A lot of tools exist, like different catheters, pads, or condom catheters. Some can help in your daily life. Some might be better suited to your lifestyle than others. If you try to explain the details of your problem, your doctor can help you select the right tools.